What Is a Ligature Point? Examples in Hospitals and Psychiatric Facilities
A ligature point is any fixed feature in a building that could be used to attach a cord, rope, belt, sheet, or other material for the purpose of hanging or strangulation. In hospitals, psychiatric wards, and correctional settings, unidentified ligature points represent one of the most serious patient safety risks a facility can face.
Understanding what constitutes a ligature point, where the most common ligature points are found, and how to reduce ligature risks through anti-ligature design is essential for anyone responsible for the safety of vulnerable patients.
Table of Contents
Why Ligature Points Matter in Healthcare and Mental Health Facilities
Ligature risks are a leading cause of inpatient suicide in psychiatric and mental health facilities. The Joint Commission estimates that between 49 and 65 inpatient suicides occur each year in the United States, and the majority of these involve hanging or strangulation using a ligature attached to a fixed point in the environment.
The risk is not limited to psychiatric wards. Patients experiencing suicidal ideation can present in emergency departments, medical-surgical units, and general hospital rooms. Any space where a patient is left unsupervised, even briefly, and where a ligature point exists, creates the possibility of self harm.
This is why healthcare facilities, mental health environments, and correctional settings are expected to conduct thorough risk assessment processes to identify and address every ligature risk in the built environment. Failing to do so can result in patient harm, regulatory citations from the Joint Commission, and in the worst cases, patient death.
What Counts as a Ligature Point?
A ligature point is defined by CMS (Centers for Medicare and Medicaid Services) as anything which could be used to attach a cord, rope, or other material for the purpose of hanging or strangulation. That definition is deliberately broad because the reality is that almost any protruding, fixed object in a room can become a ligature point under the wrong circumstances.
Common ligature points found during facility risk assessments include:
Door hardware and fittings. Door hinges, door closers, door furniture such as handles and lever sets, and the tops of doors themselves are among the most common ligature points identified by surveyors. In some cases, accreditation surveyors have tested ligature risk by hanging dental floss over door hinges to confirm whether material could be looped and secured.
Window fixtures. Window frames, window latches, window restrictors, and any hardware attached to or around a window can create a ligature point. Blinds and curtain cord fittings are also high-risk fixtures in patient spaces.
Hooks and coat hooks. Wall-mounted coat hooks, towel hooks, and robe hooks are frequently cited ligature points. Even hooks with rounded edges can still support enough weight and grip to create a ligature risk if they protrude from the wall surface.
Bathroom fittings. Shower rails, shower heads, exposed pipes, towel rails, grab bars, taps, and plumbing fixtures are all potential ligature points. Bathrooms are among the highest-risk spaces in psychiatric wards and mental health facilities because patients are often unsupervised in these areas and have access to towels, sheets, belts, and clothing that could be used as ligature material.
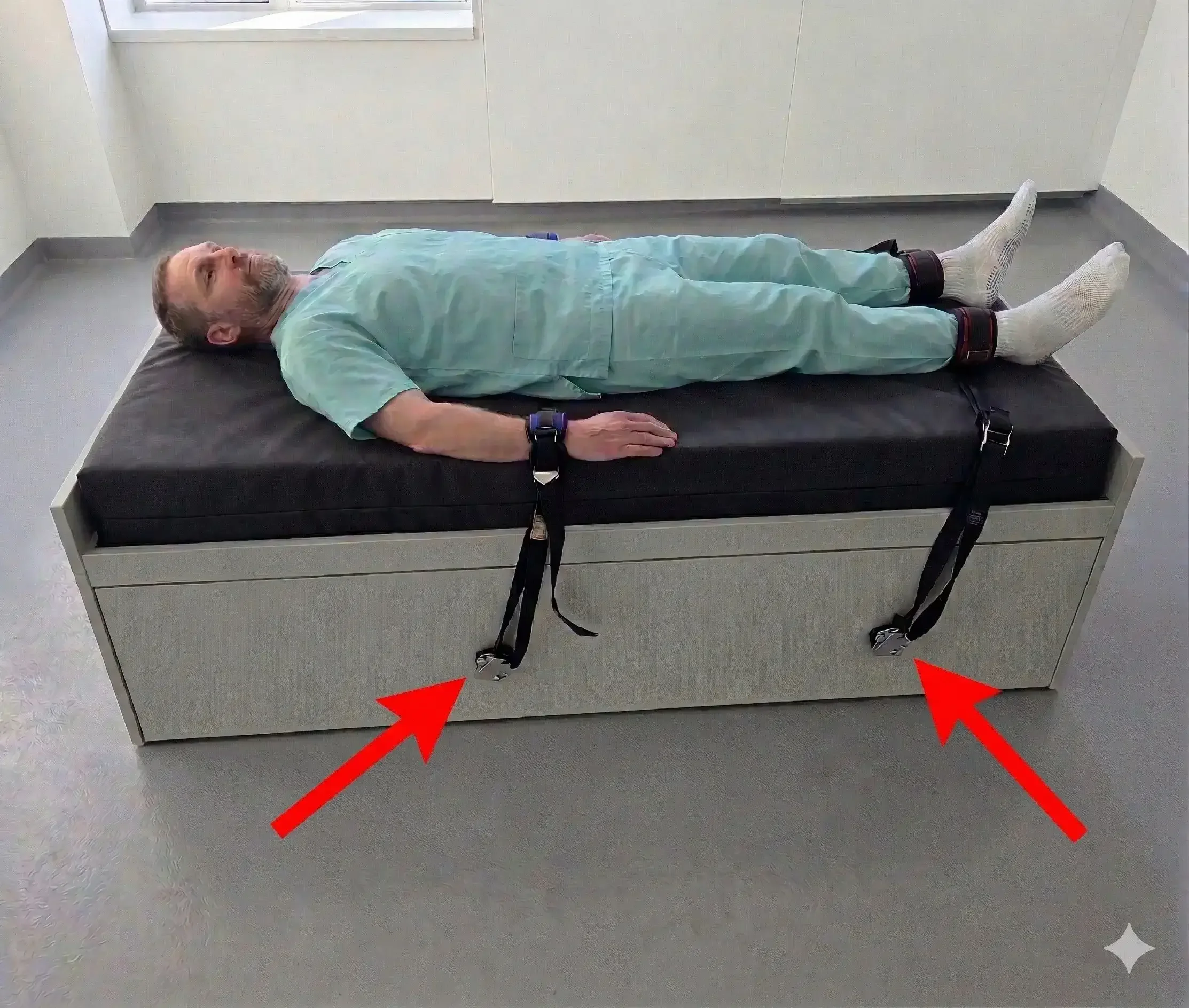
Bed frames and furniture. Bedsteads, bed rails, and furniture with exposed structural elements can all serve as anchor points. This includes the restraint attachment points on psychiatric beds, which have been specifically cited by the Joint Commission as creating ligature risks when they feature external rings or protruding hardware.
Ceiling and lighting fixtures. Ceiling-mounted light fittings, sprinkler heads, ventilation grilles, and any object attached to the ceiling can function as a ligature point if material can be looped around it.
Radiators, pipes, and utility fittings. Exposed heating pipes, radiator elements, and utility access points are common ligature risks, particularly in older facilities that were not constructed with anti-ligature design principles in mind.
Where Are Ligature Risks Most Commonly Found?
The most common ligature points in healthcare facilities tend to cluster in specific areas where two factors overlap: the patient has reduced supervision, and the environment contains fixtures and fittings that were not originally designed with safety in mind.
Patient bedrooms. Approximately 75% of inpatient suicides in psychiatric hospitals occur in bedrooms, bathrooms, or closets. Bedrooms contain multiple potential ligature points including bed frames, window hardware, door hinges, and wardrobe fittings. Any object a patient could loop sheets, clothing, belts, or towels around is a risk.
Bathrooms. Bathrooms are particularly high-risk spaces because patients are expected to have privacy, which reduces the ability for staff to maintain continuous observation. Shower fixtures, grab bars, exposed pipes, hooks, and door hardware all create ligature points. Some facilities in the UK and US have replaced bathroom doors with curtains to reduce risk, although the curtains themselves then require their own safety assessment.
Corridors and common areas. In behavioral health settings, patients spend significant time outside their rooms. Corridor fixtures, handrails, door hardware, fire equipment housings, and signage brackets can all create ligature points. Anti ligature design in these spaces is just as important as in patient rooms.
Seclusion and restraint rooms. These environments require the highest level of ligature risk management. Every fixture, fitting, and surface must be assessed. Restraint anchor points that protrude from furniture or floors when not in use represent a specific and well-documented ligature risk, one that the ERSO Restraint Anchor was engineered to address through its flush-mount design.
The Role of Anti-Ligature Design in Reducing Risk
Identifying ligature points is only the first step. The goal for designers, builders, facility managers, and healthcare professionals is to reduce and minimize ligature risks through a combination of anti ligature products, ligature resistant fixtures, and thoughtful environmental design.
Anti-ligature design focuses on eliminating protruding features, using fixtures with rounded edges that prevent material from being looped or tied, and selecting fittings constructed from materials that are both tamper resistant and easy to clean for infection control.
Key principles of anti-ligature design include:
Flush-mount hardware. Fixtures that sit flush with the wall, floor, or furniture surface when not in use minimize the opportunity for material to be attached. This principle applies to everything from door furniture to restraint anchors.
Breakaway and collapsible fittings. Some ligature resistant fixtures are designed to collapse or release under a specific weight load, reducing the risk of strangulation. Shower heads, curtain rails, and grab bars in mental health settings are commonly specified with breakaway features.
Tamper-resistant construction. Anti ligature products must be constructed using tamper-resistant fasteners and materials that prevent patients from disassembling or modifying the object to create a ligature point.
Rounded and sloped profiles. Features and fittings with aggressively rounded edges and sloped surfaces reduce the ability to loop or tie rope, cord, sheets, or clothing around them. This is a core principle applied across all anti ligature products, from hinges and hooks to furniture and door hardware.
Compliance, Standards, and the Expectation to Act
In the US, the Joint Commission and CMS set the standards that healthcare facilities are expected to meet regarding ligature risk management. The Joint Commission defines a ligature resistant environment as one "without points where a cord, rope, bedsheet, or other fabric or material can be looped or tied to create a sustainable point of attachment that may result in self harm or loss of life.”
Facilities that fail to meet national safety requirements for ligature risk face immediate citations and must submit corrective action and mitigation plans. In the UK, the NHS and CQC set equivalent guidelines, and NHS Trusts are expected to conduct regular environmental safety assessments and address identified risks promptly.
The compliance process typically involves a structured risk assessment of every space where patients may be present, followed by the development of mitigation plans that specify how each identified ligature risk will be addressed. This may involve replacing fixtures with ligature resistant alternatives, modifying the environment to remove or reduce ligature points, or implementing enhanced supervision protocols in settings where full ligature resistance has not yet been achieved.
For architects, designers, builders, and facility safety teams, the focus should always be on specifying anti-ligature products and ligature resistant fixtures from the outset, whether in new construction or retrofit projects. Purpose-built solutions, like the ERSO Restraint Anchor, are designed to integrate into furniture, floors, and walls while eliminating the ligature point entirely when not in clinical use.
Ligature Risk Is an Ongoing Management Process
It is important to recognize that achieving a ligature resistant environment is not a one-time project. Environments change. New furniture is introduced, fittings wear, and patient populations shift. Routine inspection, staff training, and periodic reassessment are all essential practices in maintaining a safe environment.
Facilities should ensure that all staff are trained to identify potential ligature points during their daily rounds and that any new feature, fitting, or piece of furniture introduced into a patient area is assessed for ligature risk before it is put into use. Contraband screening for items such as belts, shoelaces, sheets, and towels that could be used as ligature material remains a critical safety practice alongside environmental management.
The most effective approach combines anti-ligature design with robust clinical practices, creating spaces that minimize environmental risk while supporting therapeutic care.
The ERSO Restraint Anchor is the only US patented, flush-mount, anti-ligature restraint anchor engineered to eliminate the ligature point created by traditional bed restraint hardware. To learn more about how it works and where it can be installed, view the product page or contact our team.
Frequently Asked Questions
-
A ligature point is any fixed object or feature in a room or facility that could be used to attach a cord, rope, belt, sheet, or other material for the purpose of hanging or self harm through strangulation. Common examples include door handles, hooks, shower rails, bed frames, window fittings, and exposed pipes.
-
The most common ligature points found in hospitals and psychiatric facilities include door hinges and handles, coat hooks, shower rails, bed frames, window hardware, exposed pipes, ceiling fixtures, and grab bars in bathrooms. Any protruding object that allows material to be looped or tied around it is a potential ligature risk.
-
Facility managers, safety officers, engineering directors, and clinical leadership teams are all responsible for conducting ligature risk assessments and implementing mitigation plans. The Joint Commission and CMS require healthcare facilities to maintain a safe environment and address identified ligature risks promptly.
-
Ligature points can be reduced by replacing standard fixtures with ligature resistant alternatives, specifying anti ligature products during new construction or renovation, conducting regular environmental risk assessments, and training staff to identify and report new risks. Purpose-built anti ligature hardware, such as the ERSO Restraint Anchor, is designed to eliminate specific ligature points associated with patient restraint systems.