How to Conduct a Ligature Risk Assessment in Hospitals
A ligature risk assessment is a structured process used to identify, evaluate, and address environmental risks that could enable patients to harm themselves through hanging or strangulation. For hospitals, psychiatric units, and behavioral health environments, conducting thorough and recurring ligature risk assessments is not optional.
It is a regulatory requirement set by the Centers for Medicare and Medicaid Services (CMS) and a core expectation of The Joint Commission's accreditation standards.
Despite this, many facilities still face challenges when it comes to knowing exactly how to conduct a ligature risk assessment, what to look for, which spaces to prioritise, and how to turn findings into actionable mitigation plans. This guide walks through the essential steps that facility managers, safety officers, and engineering directors should follow to ensure their environments are as safe as possible for patients and staff.
Table of Contents
Why Ligature Risk Assessments Matter
Suicide and self harm remain among the most serious patient safety concerns in healthcare settings. The Joint Commission estimates that 49 to 65 inpatient suicides occur annually in the United States, and research consistently shows that approximately 77% of suicides on psychiatric wards involve hanging. Given that many suicide attempts in clinical environments are impulsive, reducing the environmental opportunity for self harm is critical to saving life.
Any observable ligature risk, no matter how small, is treated as an immediate Recommendation for Improvement (RFI) when identified during an accreditation survey of an inpatient psychiatric area. Facilities must correct these findings within 45 days or less depending on severity. Failing to conduct regular assessments, or failing to act on findings, places patients at risk, exposes the facility to compliance failures, and can result in the loss of Medicare and Medicaid certification.
The focus for achieving a ligature resistant environment is primarily aimed at locked psychiatric units of acute care hospitals and psychiatric hospitals. CMS also expects hospitals to protect patients at risk of suicide or self harm in non-psychiatric settings, including emergency departments and medical-surgical units, through appropriate monitoring, environmental risk identification, and mitigation.
Step 1: Assemble a Multidisciplinary Assessment Team
A ligature risk assessment should never be conducted by a single person working in isolation. The process benefits from collaboration between professionals with different perspectives on the care environment. An effective assessment team typically includes facility managers or engineering directors, clinical nursing staff from the unit being assessed, infection control specialists, patient safety officers, and where possible, architects or design consultants with experience in behavioral health environments.
Each person on the team brings a different focus. Clinical staff understand how patients interact with the space. Facilities staff understand the construction and hardware in each room. Safety officers understand the regulations and compliance requirements. This collaboration ensures that assessments are comprehensive and that nothing is overlooked.
Step 2: Define the Scope and Priority Areas
Not every space in a hospital carries the same level of ligature risk, and the assessment process should reflect this. CMS and The Joint Commission require that inpatient psychiatric units achieve a fully ligature resistant environment in patient bedrooms, bathrooms, corridors, and common patient care areas.
Beyond psychiatric units, hospitals must also assess environments where patients at risk of suicide may receive care. This includes emergency departments, intensive care units, and medical-surgical rooms. In these non-psychiatric settings, the goal is not full ligature resistance but rather staff awareness and proactive mitigation of environmental risks when a high-risk patient is present.
When planning the scope of a risk assessment, prioritise the spaces where patients are most likely to be unsupervised. Studies consistently identify bedrooms and bathrooms as the highest-risk areas, as these are the spaces where patients spend time alone and where monitoring is most difficult. Corridors, common rooms, seclusion rooms, and outdoor areas accessible to patients should also be included.
Step 3: Conduct a Room-by-Room Physical Inspection
The physical inspection is the core of the ligature risk assessment process. This involves a systematic, room-by-room review of every fixture, fitting, and structural feature that could serve as a potential ligature point.
In each room, the assessment team should examine the following:
Doors. Inspect hinges, handles, closers, and the gap between the door and frame. Assess whether the top of the door could be used as an anchor point. Doors are one of the most frequently cited ligature risks in psychiatric units and general hospital rooms alike.
Bathrooms. Inspect shower fixtures, grab bars, towel rails, exposed pipes, taps, and toilet hardware. Bathrooms are among the most dangerous spaces in any facility because patients are often unsupervised and have access to materials such as towels and clothing that could be used as ligature material. Every fixture in a patient bathroom must be assessed.
Windows. Check window frames, handles, restrictors, and any hardware attached to the window. Blinds and curtain cord fixtures are common ligature risks that are often missed during initial assessments.
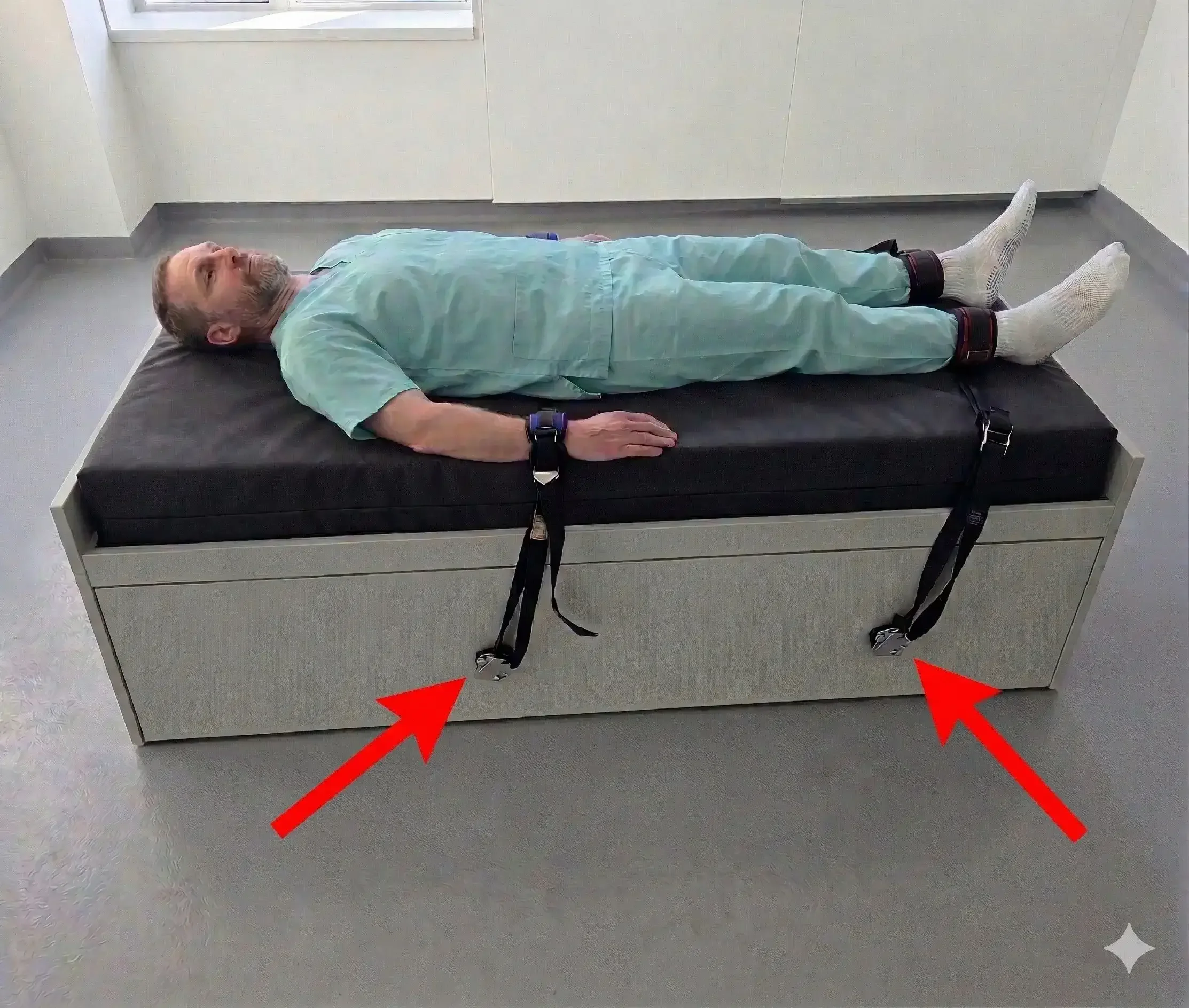
Furniture and beds. Examine bed frames, headboards, side rails, and any exposed structural elements. Pay particular attention to restraint attachment points on psychiatric beds. External rings and protruding hardware used for patient restraint have been specifically cited by The Joint Commission as creating ligature risks, which is a compliance gap the ERSO Restraint Anchor was designed to address.
Ceiling and wall fixtures. Inspect light fittings, sprinkler heads, ventilation grilles, HVAC covers, and any wall-mounted fixtures including hooks, handrails, and signage brackets.
Utility infrastructure. Check for exposed pipes, radiators, electrical conduit, and cable trays. Older facilities constructed before current safety standards were in place often have significant environmental risks in these areas.
Use a standardized checklist or assessment tool for each room. While CMS does not mandate a specific tool, organizations such as ASHE (American Society for Healthcare Engineering) have published ligature identification checklists covering 39 common ligature points that hospitals can use as a starting framework. The VA Mental Health Environment of Care Checklist is another widely referenced tool.
Step 4: Score and Prioritize Each Risk
Once the physical inspection is complete, each identified risk must be scored and prioritized. Not all ligature risks carry the same level of severity, and the assessment should reflect this by assigning a risk rating to each finding.
A practical approach is to rate each risk based on two factors: the likelihood that a patient could use the fixture as a ligature point, and the potential severity of harm if they did. Fixtures in unsupervised areas such as bedrooms and bathrooms will typically score higher than those in continually supervised common spaces.
The output of this step is a ranked list of ligature risks that allows the facility to direct resources toward the most critical issues first. This prioritization is essential because most hospitals cannot remediate every finding simultaneously, and regulators understand this. What matters is that the facility can demonstrate a clear, documented process for identifying risks, prioritizing them, and working through remediation in a structured way.
Step 5: Develop and Document Mitigation Plans
For every identified ligature risk, the facility must develop a mitigation plan. Mitigation can take several forms depending on the nature of the risk and the environment.
Replace fixtures with ligature resistant alternatives. This is the most direct and effective step. Replacing standard door hardware, shower fixtures, grab bars, hooks, and bed hardware with purpose-built ligature resistant products eliminates the risk at its source. For restraint anchor points specifically, the ERSO Restraint Anchor provides a flush-mount, spring-loaded solution that removes the ligature point entirely when not in clinical use.
Remove unnecessary fixtures. In some cases, the simplest mitigation is removal. Coat hooks, towel bars, and non-essential fittings in patient areas can often be removed without affecting the care environment.
Implement enhanced monitoring. In environments where full ligature resistance has not yet been achieved, CMS requires that patients at high risk of suicide receive continuous 1:1 observation by a qualified staff member who can intervene immediately. Video monitoring alone is not considered sufficient. This approach is often used as an interim measure while physical remediation is underway.
Restrict patient access. If a specific room or area contains unmitigated ligature risks, patients should be restricted from that space until the risks have been addressed. This is particularly important in cases where a restraint anchor has failed to close or lock properly after use.
Each mitigation plan must be documented, including the specific risk, the planned action, the responsible person, and the timeline for completion. CMS and The Joint Commission expect hospitals to maintain this documentation and to be able to produce it during surveys.
Step 6: Implement Staff Training
A ligature risk assessment is only as effective as the staff who act on it. All clinical and facilities staff should receive regular training on identifying ligature risks, responding to incidents of self harm, and understanding the facility's mitigation plans.
Staff training should cover how to recognise potential ligature points during daily rounds, how to conduct a bedside environmental sweep before placing a high-risk patient in a room, and the correct procedures for reporting new or emerging risks. In facilities that use restraint systems, staff must also be trained on the correct operation and inspection of restraint hardware, including verifying that anchors are fully closed and locked after every restraint period.
Training should not be a one-time exercise. It must be conducted regularly, updated when regulations change or new fixtures are introduced, and documented to demonstrate compliance during accreditation surveys.
Step 7: Schedule Ongoing Assessments and Updates
Assessments are not a one-off compliance task. Environments change over time. New furniture is introduced, fixtures wear and degrade, renovation projects alter room layouts, and patient populations shift. Each of these changes can introduce new ligature risks that were not present during the previous assessment.
CMS expects hospitals to maintain documentation of their environmental risk assessments and to conduct them on a recurring basis. Many facilities schedule formal assessments quarterly, with informal environmental checks conducted at each shift change. The Joint Commission also expects that ligature risk mitigation is incorporated into the facility's quality assessment and performance improvement program, ensuring that the process is treated as an ongoing management responsibility rather than a periodic compliance exercise.
Any time a new product, fixture, or piece of furniture is introduced into a patient care area, it should be assessed for ligature risk before it enters service. This includes beds, chairs, hardware, and any retrofit installations. Environmental rounds by facilities staff should include a specific focus on verifying that previously remediated risks remain addressed and that no new risks have emerged.
The Connection Between Risk Assessment and Product Specification
One of the most valuable outcomes of a thorough ligature risk assessment is that it provides the evidence base for specifying the right products. When a facility identifies that its restraint bed hardware creates an external ligature point, the assessment documents the risk, and the mitigation plan defines the solution.
This is exactly the compliance gap that the ERSO Restraint Anchor was engineered to close. By replacing exposed restraint rings with a flush-mount, spring-loaded anchor that retracts and locks when not in use, the ERSO product directly addresses one of the most commonly cited ligature risks in behavioral health and correctional environments. Facilities that conduct regular ligature risk assessments and act on their findings are better positioned to protect patients, maintain compliance, and provide care in environments that support recovery rather than compromise safety.
The ERSO Restraint Anchor is the only US patented anti ligature restraint anchor designed to eliminate the ligature point created by traditional bed restraint hardware. To learn more about specifications and installation methods, view the product page or contact our team.
Frequently Asked Questions
-
A ligature risk assessment is a structured process used to identify fixtures, fittings, and structural features in a healthcare environment that could be used by patients as anchor points for hanging or strangulation. Hospitals, psychiatric units, and behavioral health facilities are required to conduct these assessments regularly to comply with CMS and Joint Commission standards.
-
CMS expects hospitals to conduct ligature risk assessments on a recurring basis and to maintain documentation of all findings and mitigation plans. Many facilities conduct formal assessments quarterly, with informal environmental checks at each shift change. Assessments should also be repeated whenever new furniture, fixtures, or hardware is introduced into a patient care area.
-
Ligature risk assessments should be conducted by a multidisciplinary team that includes facility managers, clinical nursing staff, patient safety officers, and where possible, architects or design consultants with experience in behavioral health environments. Collaboration ensures that both clinical and environmental risks are identified.
-
Any ligature risk identified in an inpatient psychiatric area during a Joint Commission survey is treated as an immediate Recommendation for Improvement. The facility must submit corrective action plans and complete remediation within 45 days or less depending on the severity and number of findings. Unresolved ligature risks can lead to loss of accreditation and Medicare and Medicaid certification.